When you take two or more sedating medications together, the result isn’t just added up-it’s multiplied. This isn’t a guess. It’s science. And it’s killing people.
Think about it: one pill makes you drowsy. Another makes you sleepy. So you take both, thinking it’ll help you sleep better or calm your nerves. But what you don’t realize is that these drugs don’t just work side by side-they team up. And when they do, they can shut down your breathing without warning.
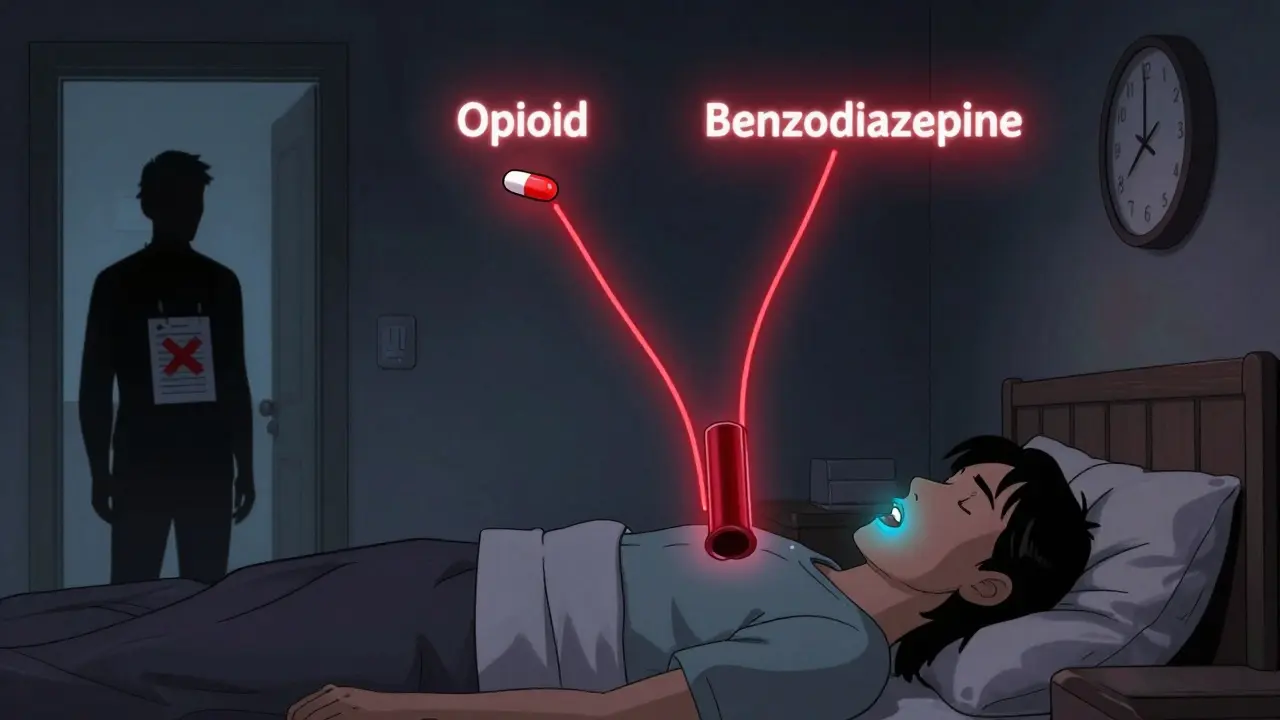
The most dangerous mix? Opioids and benzodiazepines. These are commonly prescribed together-opioids for pain, benzodiazepines for anxiety or insomnia. But the data doesn’t lie. According to the Centers for Disease Control and Prevention (CDC), in 2020, nearly 1 in 6 opioid-related overdose deaths also involved a benzodiazepine. That’s not coincidence. That’s a direct, predictable outcome of how these drugs interact in your brain.
How Sedating Medications Work Together
All sedating medications-whether they’re prescription sleep aids like zolpidem (Ambien), anti-anxiety drugs like alprazolam (Xanax), painkillers like oxycodone, or even alcohol-work by slowing down your central nervous system. They boost the effect of a brain chemical called GABA, which tells your brain to relax. When one drug does this, it’s manageable. When two or more do it at the same time, your brain gets overwhelmed.
This isn’t additive. It’s synergistic. That means the combined effect is greater than the sum of each part. A 2017 study in JAMA Internal Medicine found that people taking both opioids and benzodiazepines had a 154% higher risk of overdose than those taking opioids alone. The odds ratio? 2.54. In plain terms: if you’re on both, you’re more than two and a half times more likely to stop breathing.
Here’s why: opioids suppress the part of your brainstem that controls breathing. Benzodiazepines amplify GABA activity, which further calms that area. Together, they can reduce your breathing rate to fewer than 8 breaths per minute. Normal is 12 to 20. Below 12, you’re in danger. Below 8, your body starts shutting down. Oxygen levels drop. Your brain starves. And you might not even realize it’s happening.
The Most Dangerous Combinations
Not all combinations are equal. Some are deadlier than others.
- Opioids + Benzodiazepines: This is the deadliest combo. UCLA Health reports it accounts for 30% of all prescription medication-related deaths. The risk of fatal overdose jumps by more than 3.8 times when both are taken together.
- Alcohol + Sedatives: Alcohol is a sedative too. Mixing it with sleep pills, anti-anxiety meds, or even antihistamines can cut your reaction time by 70%. That’s why falls, car crashes, and blackouts are so common. American Addiction Centers found that just two drinks with a standard dose of Ambien can make you as impaired as someone with a blood alcohol level of 0.15%-well above the legal driving limit.
- SSRIs + MAOIs: These are antidepressants, but when combined, they can trigger serotonin syndrome. It’s rare, but deadly. Too much serotonin floods your nervous system. Symptoms: high fever, rapid heartbeat, muscle rigidity, confusion. In severe cases, it can cause seizures or organ failure. About 14-16% of cases require hospitalization.
- Benzodiazepines + Antipsychotics: Used together for severe mental health conditions, but they increase the risk of dizziness, falls, and sudden drops in blood pressure. Older adults are especially vulnerable.
And here’s the scary part: you might not even know you’re taking a dangerous mix. Many people don’t realize that over-the-counter sleep aids like diphenhydramine (Benadryl) are sedating. Or that some cough syrups contain dextromethorphan, which can worsen respiratory depression when combined with opioids.
Warning Signs You Can’t Ignore
Most overdoses don’t happen suddenly. They creep up. You start feeling off. But you blame it on stress, aging, or just being tired.
Here’s what to watch for-especially if you’re on more than one sedating drug:
- Shallow or slow breathing (fewer than 12 breaths per minute)
- Unresponsiveness-you can’t wake someone up with loud voice or shoulder shake
- Blue lips or fingertips (sign of low oxygen)
- Extreme confusion or slurred speech that’s worse than usual
- Gurgling sounds while sleeping (a sign of airway blockage from muscle relaxation)
- Unexplained falls or injuries
If you or someone you know shows even one of these signs, call emergency services immediately. Don’t wait. Don’t assume they’ll “sleep it off.” This isn’t sleep. This is respiratory failure.

Who’s at Highest Risk?
It’s not just people who misuse drugs. Many victims are older adults on multiple prescriptions.
The American Geriatrics Society Beers Criteria lists 53 medication combinations that older adults should avoid. Nineteen of them involve sedating drugs. Why? Because aging slows how your body processes medications. Your liver and kidneys don’t clear them as fast. So even normal doses build up. And if you’re over 65 and taking three or more sedatives? Your risk of falling increases by 50%.
Women are more likely than men to be prescribed these combinations. One study found 41% of older women were on potentially inappropriate sedatives, compared to 27% of men. Why? Anxiety and insomnia are more commonly diagnosed in women-and more often treated with benzodiazepines or sleep aids.
And then there’s the hidden problem: doctor shopping. Recovery Village data from 2022 shows that 42% of people who overdosed on combined sedatives had gotten prescriptions from three or more doctors in just six months. They weren’t addicts. They were confused patients trying to manage pain, anxiety, and sleep-all at once-without realizing the risks.
What You Can Do to Stay Safe
You don’t have to live in fear. But you do need to be informed.
1. Know every medication you’re taking. That includes prescriptions, over-the-counter pills, herbal supplements, and even alcohol. Write them down. Keep the list on your phone and in your wallet.
2. Ask your doctor or pharmacist: “Could any of these drugs interact?” Don’t assume they’ll catch it. A 2020 study in JAMA Network Open found that only 17.3% of dangerous combinations triggered alerts in electronic health records. Systems aren’t perfect. You have to be.
3. Never mix alcohol with sedatives. Not even one drink. The interaction is unpredictable, and the margin between “feeling relaxed” and “stopping breathing” is razor-thin.
4. Get a medication review every 3 months. Especially if you’re over 65. The START criteria recommend a full reassessment if you’re on three or more sedating drugs. Many side effects-dizziness, confusion, weakness-can be fixed by adjusting one pill.
5. Learn morphine milligram equivalents (MME). If you’re on opioids, know how strong they are. The CDC recommends keeping daily MME below 50 mg. Above that, risk rises sharply. Above 90 mg? Your overdose risk doubles.
6. If you’re being prescribed a new sedative, ask: “Is this absolutely necessary?” Often, there are non-sedating alternatives. For anxiety, therapy and SSRIs work better long-term than benzodiazepines. For sleep, cognitive behavioral therapy (CBT-I) is more effective than pills.
What’s Being Done-and What’s Not
The FDA now requires boxed warnings on all opioid and benzodiazepine labels. All 50 states require electronic prescribing for controlled substances, which includes checks for dangerous combinations. The CDC’s 2022 guidelines say: avoid prescribing opioids and benzodiazepines together unless absolutely necessary.
But here’s the gap: only 28% of primary care providers consistently screen for these interactions. And the cost of safer alternatives? A non-sedating antidepressant can cost $450 a month. A benzodiazepine? $15. For low-income patients, the choice isn’t about safety-it’s about affordability.
There’s hope. The FDA’s DETERMINE platform, launched in 2022, uses AI to predict individual risk of sedative interactions with 87.4% accuracy. And the NIH is investing $127 million into pharmacogenomic testing-blood tests that can tell if your body is genetically prone to bad reactions with certain drugs.
But until those tools are standard, your awareness is your best defense.
When It’s Too Late
Some people don’t realize they’re in danger until it’s too late. A Reddit user from Perth wrote in March 2023: “I took my sleep med and had two glasses of wine. Woke up on the floor. Couldn’t remember how I got there. My husband had to carry me to bed.” That’s not a one-off. It’s a pattern.
Don’t wait for a crisis. If you’re on multiple sedating drugs, talk to your doctor today. Ask for a full review. Ask if you can taper one down. Ask about alternatives. Your life isn’t worth the risk of a silent, invisible overdose.
Can combining sedating medications be safe under medical supervision?
In very rare cases, yes-but only under strict, ongoing monitoring by a specialist. For example, some patients with severe treatment-resistant anxiety or chronic pain may be prescribed a low-dose combination, but only after multiple failed alternatives. Even then, dosages are kept as low as possible, and patients are monitored weekly for signs of respiratory depression or cognitive decline. The American Geriatrics Society and FDA both warn that this should be the exception, not the rule.
What should I do if I think I’m taking too many sedating drugs?
Stop taking any new or unnecessary medications immediately. Then schedule a full medication review with your doctor or pharmacist. Bring a list of everything you take-including supplements, alcohol, and recreational drugs. Ask specifically: "Which of these could be interacting?" Do not stop benzodiazepines or opioids abruptly-this can cause seizures or dangerous withdrawal. Tapering must be done slowly under medical supervision.
Are over-the-counter sleep aids safe to combine with prescription sedatives?
No. Many OTC sleep aids like diphenhydramine (Benadryl) or doxylamine (Unisom) are potent CNS depressants. When combined with prescription sleep meds like zolpidem or benzodiazepines, they can cause extreme drowsiness, memory loss, and respiratory depression. A 2021 study found that 31% of older adults who overdosed on sleep medications had used OTC products alongside their prescriptions.
Why do some people feel better when they combine sedatives?
Some people report feeling more relaxed or sleeping better when combining sedatives because the effects are amplified. But this is temporary and misleading. The body builds tolerance quickly, meaning you’ll need higher doses over time to get the same effect. This increases risk exponentially. What feels like improvement is actually the beginning of dependence and escalating danger.
Can I just reduce my dose on my own?
No. Reducing sedating medications without medical supervision can be dangerous. Benzodiazepines and opioids can cause life-threatening withdrawal symptoms, including seizures, hallucinations, and rebound anxiety. Always work with a doctor to create a tapering plan. Typically, doses are reduced by 10-25% every 1-2 weeks, depending on the drug and your health. Never skip this step.
How can I tell if a medication is sedating?
Check the label. Look for words like "may cause drowsiness," "use with caution if operating machinery," or "avoid alcohol." Common sedating drugs include benzodiazepines (Xanax, Valium), sleep aids (Ambien, Lunesta), opioids (oxycodone, hydrocodone), muscle relaxants (cyclobenzaprine), antihistamines (Benadryl), and some antidepressants (trazodone, mirtazapine). If you’re unsure, ask your pharmacist.










11 Comments
Bro, I took Xanax and melatonin last night after a bad day. Woke up on the floor. No idea how. My dog was licking my face like I was a lost snack. 🤯 That’s not sleep. That’s a near-death experience with a side of fur. Don’t be that guy.
I’ve been on three sedatives for anxiety and chronic pain for five years. I didn’t realize how much I was teetering until I started forgetting my own birthday. Not joking. I thought my cat was my sister. The doctor finally sat me down and said, ‘You’re not managing your life-you’re just surviving on chemical fog.’ I’ve cut two of them out. Not perfect. But I can remember my kid’s name again. That’s worth more than any pill.
Y’all need to stop treating meds like candy. I used to be the guy who’d say, ‘Oh, just take an extra one if you’re still awake.’ Then my uncle OD’d on a combo of oxycodone and Ambien. He didn’t even get a warning label. His doctor didn’t even ask if he drank. We lost him because we thought it was ‘just a little help.’ Don’t wait for a funeral to get smart. Talk to your pharmacist. They’re the real heroes.
The CDC? FDA? They’re all part of the pharmaceutical deep state. They want you scared so you keep buying pills. Real solution? Stop taking anything. Go live in the woods. Breathe. Meditate. The system is rigged to keep you dependent. They don’t want you well. They want you medicated. I know. I worked in a pharmacy. The numbers don’t lie… but neither do the secrets.
i think the real issue is that doctors are lazy and dont wanna deal with therapy or cbt so they just write scripts like its a vending machine. also why is everyone so scared of alcohol? its just water with vibes. i had 2 glasses with my sleep med and i just slept harder. no big deal. maybe im just built different lol
I’ve been tracking every pill I take since my sister died from a 'accidental overdose'... and I swear, the government is watching. I think they’re using the EHR system to push people into fatal combos. I’ve been told to take 3 different sedatives... but I’ve been recording every interaction on a spreadsheet. If you’re on more than two, you’re already in a lab. I’m not paranoid-I’m prepared.
In India, we don’t have this problem as much-not because we’re smarter, but because most people can’t afford five prescriptions. We use turmeric, yoga, and chai. But I’ve seen Western friends here take 7 pills before bed and wonder why they wake up confused. It’s not magic. It’s physics. Your brain isn’t a video game where you stack power-ups. It’s a fragile machine. Treat it like one.
I used to think I was just 'a heavy sleeper' until I woke up with my phone in my mouth and my cat on my chest. I had taken Benadryl, melatonin, and my anxiety med. I didn’t even know Benadryl was a sedative. I thought it was just for allergies. My pharmacist laughed when I told her. She said, 'Sweetie, that’s basically sleeping potion with a side of confusion.' I’ve cut it all out. Now I read before bed. It’s slower. But I remember my dreams. And I remember my life.
If you’re combining sedatives, you’re not sick. You’re stupid.
Oh wow, another article that says 'drugs are dangerous' like we didn’t already know. The real problem? No one tells you how to get off them. You get prescribed 3 sedatives, then 5 years later, you’re addicted and no doc will touch you. They say 'just taper' like it’s easy. Try quitting Xanax cold turkey after 3 years. Go ahead. I dare you. Meanwhile, the system keeps churning out new prescriptions like it’s Black Friday. And yeah, CBT-I works. But it costs $200 a session. What’s a low-income person supposed to do? Starve? That’s not healthcare. That’s capitalism with a stethoscope.
I’m 72. Took 4 meds for sleep and pain. Didn’t realize I was walking like a drunk until my grandson said, 'Grandpa, why are you doing the robot?' Cut one. Then another. Now I nap for 20 minutes. Walk 10 minutes. Sleep like a baby. No pills. Just routine. It’s not sexy. But it’s real.